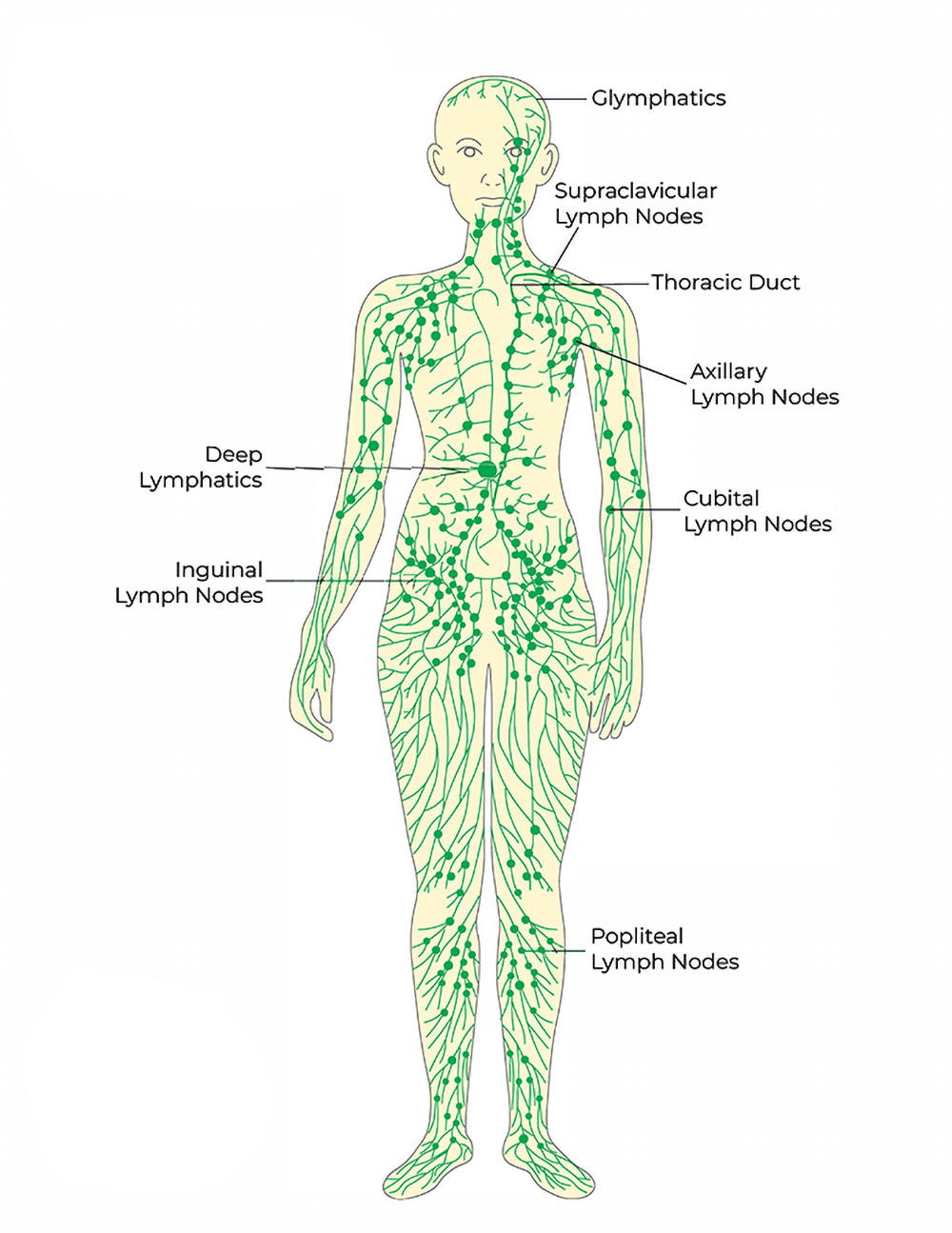
What is lymphedema?
Lymphedema is a condition where lymphatic fluid builds up under the skin, causing swelling. This often happens in the arms or legs, but it can also affect areas like the chest, trunk, head, neck, and genitals. Lymphedema can be managed well through early identification, early treatment, and following treatment recommendations.
It occurs when the lymphatic system—which normally drains fluid and filters waste—doesn’t work properly. For individuals with spinal cord injury, this can happen due to reduced muscle activity, trauma, surgery, or other conditions such as deep vein thrombosis or heart failure.
The lymphatic system is part of your immune system and helps remove waste and toxins from your body. When lymphedema isn’t managed, it can lead to skin infections, pain, heavier limbs, and may even slow neurological recovery.
There are two types of lymphedema:
- Primary lymphedema: Caused by problems in the lymphatic system from birth.
- Secondary lymphedema: Caused by injury, surgery, or other conditions—common in spinal cord injury patients.